- Home
- Skin
- Fungal Infections
- Fungal Infections Treatment in Delhi
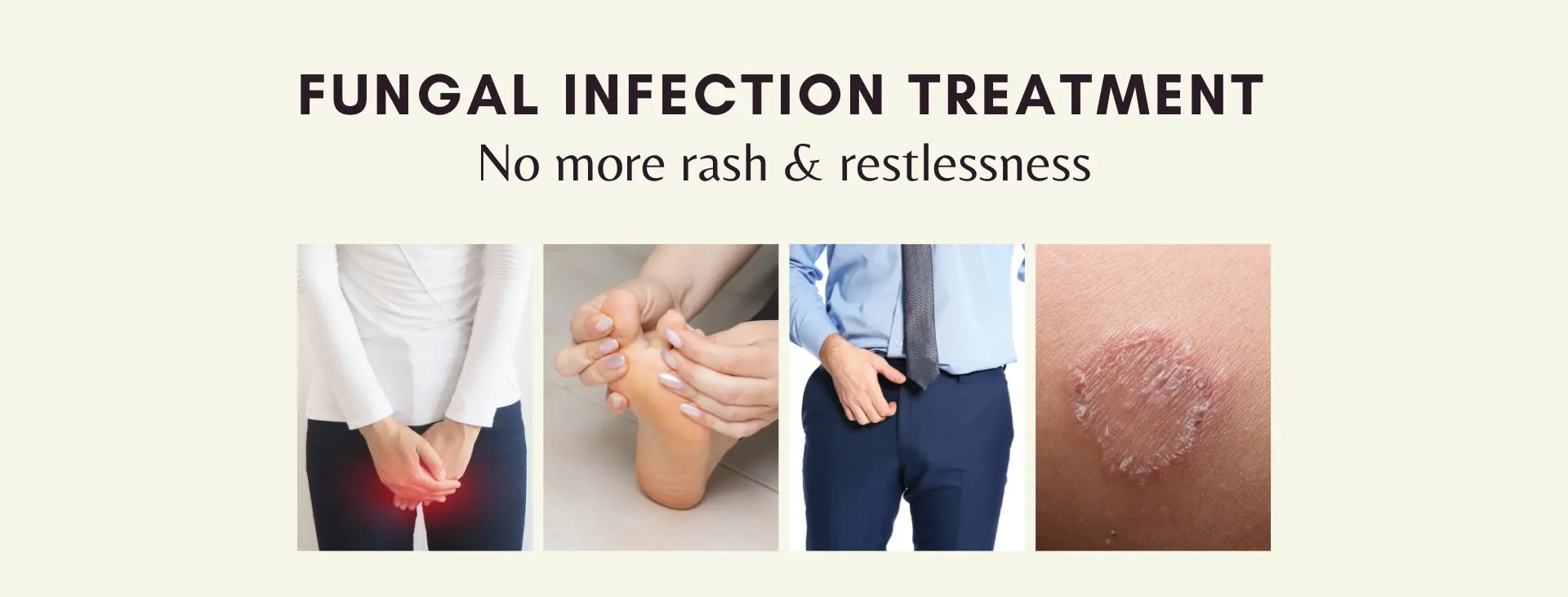
Fungal Infection Treatment
Introduction
Fungal infections are more common in warm moist environments. Skin infections caused by fungus are more common in the moist areas of the body. To prevent any allergic reactions, one must keep the infected area clean and dry.
In medical terms, rashes causing fungus are called tinea, representing ring-shaped rashes on the skin. Tinea corporis denote fungal infection covering a more significant part of the body.
Symptoms
- • Itching
- • Redness
- • Swelling
- • Scaly Skin
- • Irritation
- • Blistering
Risk Factors
Risk factors for fungal infections include,
- • Immunocompromised patients
- • A prolonged course of antibiotics
- • Chronic alcoholic
- • In babies due to diapers
- • Individuals with Exessive sweating
- • During Pregnancy
- • Overweight & Obesity
- • Uncontrolled Diabetes
Types of Fungus
There are mainly four common types of fungal infections.
1. Athletes Foot
Athletes foot is also called tinea pedis. Fungal growth occurs in warm and moist environment and hence it is more common among athletes and sports players as the prolonged wearing of the socks and shoes leads to sweating and creates a favorable environment for the fungal organisms to grow leading to fungal infection of the foot. It can be of 3 different types, namely.

• Interdigital Infection
In this the infection is in between the toe fingers. The skin appears pale and can spread to the sole of the feet. There can be some cuts and wounds in between the fingers which most likely appears after vigorous itching.
• Moccasin
When the infection spreads to the entire sole of the foot or sides, it is called moccasin. It presents with itching and cracking of the skin in between the digits of the feet.
• Vesicular
It is characterised by small fluid filled blisters on the soles of the feet and this is the rarest form of athletes foot fungal infection.
2. Yeast Infection
Vaginal yeast infection are common in females. It is due to alteration in the normal bacterial flora in the vagina which leads to overgrowth of yeast and cause vaginal fungal infections. The causative organism is cadida albicans. The alteration in the normal vaginal flora could be due to stress, hormonal imbalances, antibiotics or due to eating disorders.

3. Jock Itch
Jock itch medically known as tinea cruris is a condition in which there is growth of fungal infection in the moist areas of the body like groin, buttock and upper medial part of thighs and more common during the summer season. It is advised not to share towels as this is contagious and thrives in the clothes and other things it comes in contact with.

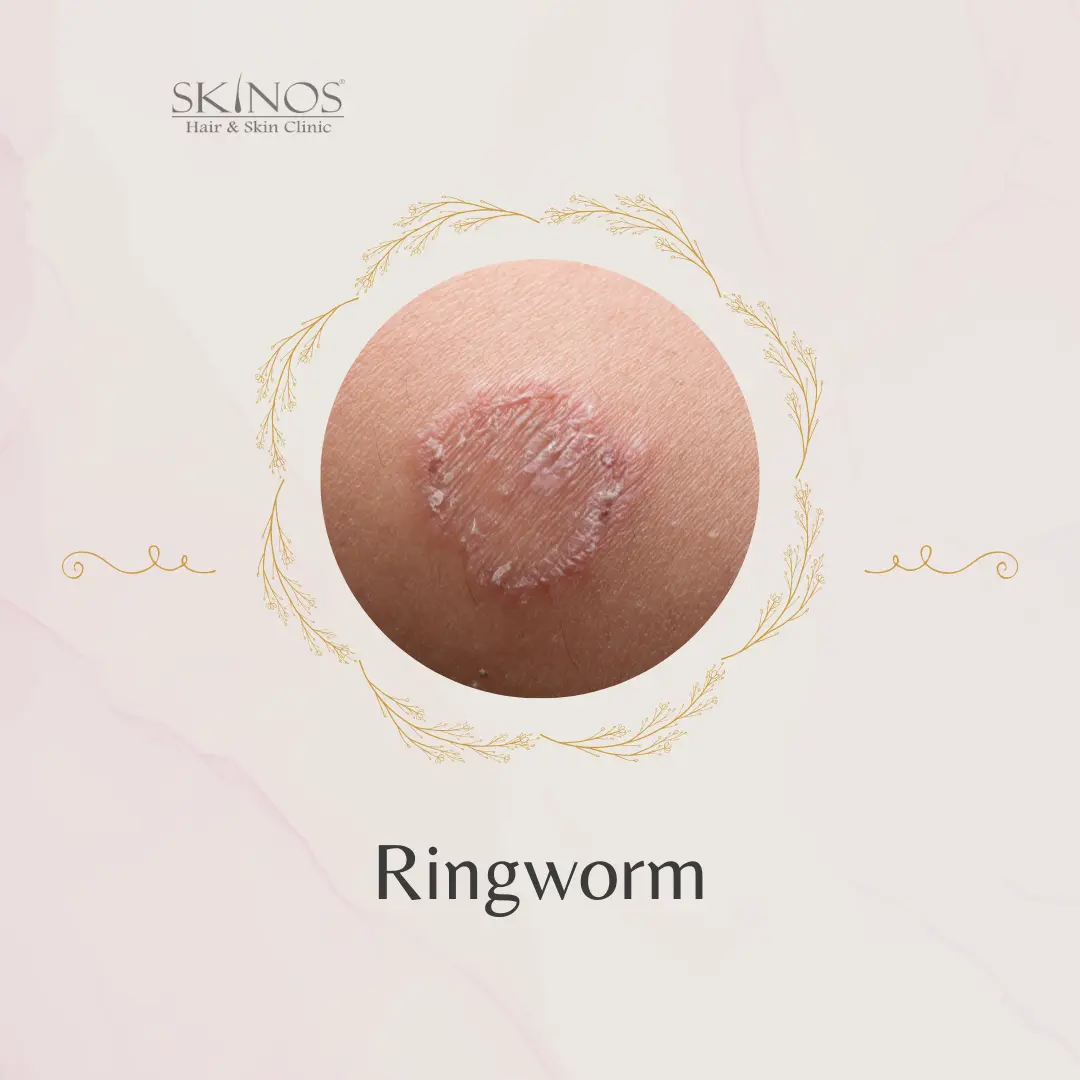
4. Ringworm
Fungal infection caused on different parts of the body other than vagina and feets are ringworm infection. It is caused by the same organism which causes tinea cruris and tinea pedis. It is ringed shaped and that is why it is named ringworm.
It is highly contagious and can survive on surfaces of towel and anything it comes in contact with including soil. It can also tramit from person to person and hence it is advisable that you consult a dermatologist at the erliest to control the progression of infection and spread to others.
5. Oral Thrush or Candida Albicans
Oral thrush is a white patch of fungal infection occurring in mouth or on tongue. It is caused by candida albicans and are called oral candidiasis.
Diagnosis and Treatment
Skin scrapping for KOH Preparation: A scrapping from the top of the rash is taken for KOH to confirm the presence of the hyphae.
Skin Biopsy for fungal Culture: A punch biopsy takes a skin sample from the affected area to identify a specific type of spores. It allows the doctor to prescribe a specific treatment tailored to that type of fungal spores for the best and most effective results.
Blood Test for severe rashes: In cases where the rashes are co-infected with bacterial organisms and fungal organisms, blood tests are required to check the severity and monitor the improvement in the treatment. Concomitant bacterial infections are common in people with weakened immune systems.
Treatment: Antifungal medications are advised after dermatologist consultation which depends on the type of fungi causing the infection. All treatments are as per American academy of dermatology guidelines. Dr.Shruti Gupta has completed her United States licensing exams and is a fellow member of AAD.
Conclusion
Fungal rashes are treatable with antifungal creams and generally do not threaten life. It can occur in any part of the body and embarrass oneself and others due to its excessive itchiness. Consulting a dermatologist helps treat the rashes and helps prevent future relapses by providing you with a list of precautions to keep you free from any fungal infections on any part of the body.
Disclaimer
This content spreads and creating awareness and educates people on fungal skin infections and should not be taken as a substitute for professional medical advice. Always consult a dermatologist before using any medication. We now disclaimer the content that it is medically reviewed for educational purposes only.
Frequently Asked Questions
A dermatologist advises that you don't self-treat and use any steroid creams to treat the fungal rash. The use of steroid creams can make the fungal infection resistant to treatment, and relapses are very common with its use. Always consult a board-certified dermatologist who is qualified to treat infectious diseases.
A dermatologist will help in fungal rash examination and diagnosis for its best medical management and treatment. Schedule your appointment today with Dr.Shruti Gupta MD, FAAD (USA), the best fungal infection treatment doctor in Delhi, India.
These are the measures advised by the center for disease control and prevention.
- • Follow the instructions by the dermatologist given to you at your visit.
- • In gyms, locker rooms, bathrooms, public showers, and carpets, do not walk barefoot.
- • Do not share your footwear with others to stop the fungal disease spread.
- • Shower after sweating to clean your skin and hair as soon as possible.
- • Keep your feet, private parts, and body cool and dry.
- • Change socks regularly and do not wear too tight footwear.
- • Keep toenails short and cut and trimmed.
- • Keep different clippers for cutting normal and infected nails.
- • Do not wear old shoes, slippers, and footwear.
- • Use antifungal powder to prevent the growth of fungal spores.
- • Use antifungal medicines and creams as advised by the doctor.
- • Use anti-dandruff shampoos regularly if you have a fungal skin infection.
It takes about 1 to 4 weeks for the fungal rash and about 1 to 4 months for nail fungal infection to show signs of improvement. However, it differs from person to person, and we advise that you consult your dermatologist to discuss the ways to prevent the spread and relapses of fungal infections that affect your skin.
A fungal rash generally presents with an uncomfortable, itchy rash. You must consult a dermatologist to prevent its spread and treat the inflammation at the earliest to avoid any complications such as,
- Development of blisters
- Development of purulent infections
- Result of fever along with the rash
You must consult in an emergency if any of the above or there is a development of widespread body rash that has occurred quickly.
Dr.Shruti Gupta, a board-certified dermatologist, consults at Skinos Hair & Skin Clinic in north Delhi. She has her MD in Dermatology from a top government medical college in India, Bangalore Medical College & Research Institute, which has many government hospitals. She has vast years of experience treating fungal-related medical conditions at government and private hospitals. She is considered the best fungal infection treatment doctor in Delhi to treat and prevent fungal infections.
Skinos is the best fungal infection treatment clinic in Delhi, owing to the high popularity and expertise of Dr.Shruti Gupta, who remains the favourite dermatologist among patients looking for skin, hair, and nail infection treatments. To schedule an appointment you may contact us at 8010-888-111 or click the link to book an appointment online.
We all understand that fungal rashes are clinical conditions and are treated with antifungal powder, creams, and oral medications. In some cases, laser treatment is indicated to control the inflammation, like nail fungal infections. The laser treatment cost for fungal infection would vary from Rs.5000 to Rs.10000 per session, depending on the area to be treated and the amount of laser shorts consumed.
What Our Patients Say
Nothing gives us more pleasure than the happiness and gratitude expressed by our clients at the end of their Skin, Hair, and Laser treatment!

I recommend Dr. Shruti Gupta because she explains everything related to my problems patiently and p...
Divya Sonkar
Student
First of all I would like to thank Dr Shruti Gupta Mam for giving me a new life. On the advice of my...
Dinesh
DU Student
Dr.Shruti is very humble and adorable to everyone she explains everything wonderfully, and answers a...
Mukta Rathee
MBBS Student
It was a pleasant experience. Your work is par above my expectations. My exuberant hair growth gives...
Mohit Shukla
DJ
I have acne issue from last 13 year's I tried all from the to homemade solution but nothing's work a...
Sonal Wahi
SQ - CA25000 +
Happy Clients
5
Qualified Doctors
9
Luxury Suites
50 +
Authorized Partners

